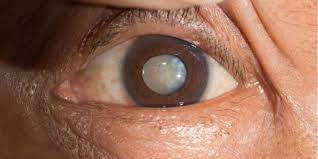
Cataract surgery has been performed successfully for decades, removing the cloudy lens and replacing it with a clear one. Cataract surgery is one of the most common procedures performed worldwide, with over 3 million procedures performed each year in the United States alone. Manual cataract surgeries in Sydney are extremely effective at restoring a patient’s vision to pre-cataract levels. According to a recent article published in the Journal of Refractive Surgery, laser cataract surgery may be even more beneficial in terms of improving vision and avoiding surgical complications.
While manual cataract surgery has an impressive 98 percent success rate in terms of major complications, one minor complication does occur in up to 30% of patients. Following manual cataract surgery, posterior capsule opacity or opacification (PCO) is a common complication. When this occurs, the growth of lens epithelial cells leftover from cataract surgery encroaches on the lens capsule’s central region. This growth of residual lens cells can eventually result in a patient’s vision deteriorating to pre-surgery levels or worsening.
To correct this issue, a laser capsulotomy is typically performed as an outpatient procedure. While this is a very low-risk procedure, it does increase the risk of retinal detachment from 1% for cataract surgery patients to 2% for capsulotomy patients. learn more about diagnosis cataracts at http://cathedralhealthcare.org/three-best-ways-of-diagnosing-cataracts/
A dislocated intraocular lens is another possible complication of a laser capsulotomy. This can result in vision problems such as double vision or a visible lens edge. To correct a lens dislocation, a second surgery is required. Additionally, infection, incision leakage, and damage to the lens’s suspensory fibers and underlying corneal cells are possible complications of surgery.
Each of these complications is less likely to occur with laser cataract surgery than with manual cataract surgery. The ophthalmologist can achieve greater accuracy and finer detail with laser equipment than with standard surgical equipment when making these tiny incisions and lens fragmentation.
New surgical techniques and laser equipment enable ophthalmologists to perform cataract surgery in a safer and more precise manner. Typically, vision is improved following cataract removal compared to prior to the formation of the cataract. The precision of the laser procedure minimizes the risk of complications such as PCO, lens dislocation, infection, and bleeding.
A recent study conducted by Dr. Kovács and published in the March issue of the Journal of Refractive Surgery demonstrated that rates of vertical lens tilt, horizontal and total decentration of intraocular lenses, and posterior capsular opacification are significantly lower with femtosecond laser cataract surgery than with standard cataract surgery. Additionally, a recent study found that an astounding 99.5 percent of respondents reported no severe complications following laser cataract surgery. Eye Physicians of Long Beach is one of the world’s first practices to offer laser cataract surgery using the Version guided system and the ORA advantage.
I’m experiencing dry eyes following cataract surgery.
Cataract surgery has been shown to exacerbate pre-existing dry eye symptoms and induce them in patients who did not have them prior to the procedure. While dry eyes can be an inconvenience, they typically last about a month following surgery and are easily treated with artificial tears (eye drops). Learn more about selecting perfect artificial tears by clicking here.
My eye is inflamed as a result of my cataract surgery.
Within two weeks of surgery, redness and swelling are common. Steroids or nonsteroidal anti-inflammatory drugs are typically used to treat inflammation (NSAIDs). If you develop inflammation following cataract surgery, your ophthalmologist will almost certainly prescribe eyedrops.
Floaters developed following cataract surgery.
Floaters are shadows cast by debris in the vitreous gel on the retina of the eye. While floaters are prevalent in many eyes, they may become more noticeable following cataract surgery as the patient’s vision improves. Consult your doctor if the floaters persist, begin to restrict your vision, or if you detect a rise in the number of floaters. This might indicate a more serious problem, such as a retinal rupture or detachment.
I am having increased sensitivity to light following cataract surgery.
Another common adverse effect is light sensitivity, which normally lasts a few days. As previously stated, cataracts can produce blurriness by filtering light entering the eye. Once this haziness dissipates, the entire world will appear brighter! Sunglasses will mitigate this impact.
While these issues are possible following surgery, the majority of them are treatable by eye physicians. Your ophthalmologist will arrange numerous follow-up sessions to check that everything heals properly and that your vision improves. If you encounter any additional issues, such as vision loss, severe pain or discomfort, or damage to your eye, you should immediately contact your ophthalmologist.
Who Should Have Surgical Procedures?
If you have a cataract, it does not always indicate that cataract surgery is necessary. You may not even realize that your eyesight has changed. Certain individuals with this syndrome can see normally if they wear prescription glasses, magnifying lenses, or utilize brighter lighting.
However, when cataracts progress, they might produce additional symptoms. You may have blurred or hazy vision. Additionally, you may have double vision when looking at objects via the cataract-affected eye. These issues might make it difficult to read, operate on a computer, or perform other tasks that need clear vision.
You may have poor night vision and hence find it more difficult to drive in the dark. You may be susceptible to headlight glare. Advanced cataract patients may potentially fail the visual portion of the driver’s exam.
Cataracts might increase your sensitivity to sunlight glare. Around strong lights, you may notice a halo. This may prevent you from spending as much time outdoors as you’d want. Additionally, it makes some activities, such as skiing or golf, more difficult to participate in.
After Surgery
Your eye may itch or feel painful for a few days following cataract surgery. You may also experience some tearing and have difficulty seeing clearly in strong light at this period.
Your doctor will prescribe eye drops to protect you from infection. You’ll need to take a few days off. Driving is prohibited, and you should avoid bending down, picking up heavy objects, or applying any pressure on your eye.
For the first week, your doctor will almost certainly recommend that you sleep with an eye shield. This shields the surgical site, allowing your eye to recuperate properly. If you have pain or believe your eye is not recovering properly, contact your doctor immediately.